[ZD18] Mortality due to respiratory diseases 

Key message

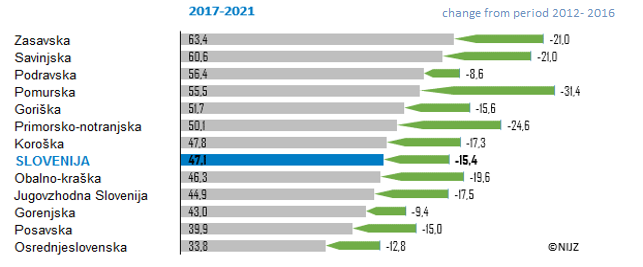
One of the main reasons of mortality due to respiratory diseases is in Slovenia chronic pulmonary disease (COPD). The highest mortality rate due to respiratory diseases in Slovenia is in Savinjska and Zasavska region and the lowest in Central-Slovenian region (2017–2021). Mortality due to respiratory diseases is decreasing; in the period 2017 to 2021 it decreased from 62/100.000 inhabitants to 32/100.000 inhabitants. This can be attributed to the “harvesting effect” of COVID 19. Because many people died due to COVID 19 in the last two years, less people died due to respiratory diseases (and other causes too).
Definition
The indicator represents mortality due to respiratory diseases in Slovenia, between 2012 and 2021, the mortality rate due to respiratory diseases by statistical regions is presented (from 2012 onwards) and the mortality rate due to respiratory diseases in European countries (for 2019).
Mortality due to respiratory diseases, which is subject to various risk factors, including polluted indoor or outdoor air. However, identification of association is not simple. Nutrition, lifestyle and other environmental and social factors can be important and also have an influence on mortality due to respiratory diseases. Mortality due to respiratory diseases is an indicator, which shows indirect assessment of exposure to adverse environmental health factors.
Charts
National Institute of Public health, 2013–2022; Statistical office of the Republic of Slovenia, 2013–2022 (1. 09. 2022)
| Eastern Slovenia[number of deaths/100.000 residents] | West Slovenia[number of deaths/100.000 residents] | Slovenia[number of deaths/100.000 residents] | |
|---|---|---|---|
| 1999 | 88.70 | 66.60 | 78.60 |
| 2000 | 77.50 | 69.60 | 73.90 |
| 2001 | 69 | 65 | 67.20 |
| 2002 | 74.50 | 65.80 | 70.50 |
| 2003 | 84.80 | 71.40 | 78.60 |
| 2004 | 80.10 | 64.90 | 73.11 |
| 2005 | 75.30 | 63.50 | 69.91 |
| 2006 | 64.20 | 58.50 | 61.60 |
| 2007 | 54.80 | 49.60 | 52.40 |
| 2008 | 59.70 | 52.30 | 56.20 |
| 2009 | 70.41 | 59.86 | 61.84 |
| 2010 | 69.86 | 53.29 | 54.61 |
| 2011 | 68.44 | 52.60 | 58.32 |
| 2012 | 75.64 | 65.49 | 67.40 |
| 2013 | 76.97 | 59.65 | 64.83 |
| 2014 | 68.68 | 50.19 | 55.88 |
| 2015 | 68.85 | 59.39 | 63.30 |
| 2016 | 69.22 | 55.64 | 61.33 |
| 2017 | 69.40 | 53.61 | 61.90 |
| 2018 | 61.10 | 42.22 | 52.20 |
| 2019 | 57.20 | 50.60 | 51.50 |
| 2020 | 43.10 | 32.60 | 38.09 |
| 2021 | 38.70 | 24.30 | 31.85 |
National Institute of Public health, 2013–2022; Statistical office of the Republic of Slovenia, 2013–2022 (1. 09. 2022)
| Gorenjska [number of deaths/100.000 residents] | Goriška [number of deaths/100.000 residents] | Jugovzhodna Slovenija [number of deaths/100.000 residents] | Koroška [number of deaths/100.000 residents] | Primorsko-notranjska [number of deaths/100.000 residents] | Obalno-kraška [number of deaths/100.000 residents] | Osrednjeslovenska [number of deaths/100.000 residents] | Podravska [number of deaths/100.000 residents] | Pomurska [number of deaths/100.000 residents] | Savinjska [number of deaths/100.000 residents] | Posavska [number of deaths/100.000 residents] | Zasavska [number of deaths/100.000 residents] | Slovenija [number of deaths/100.000 residents] | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2017-2021 | 43.04 | 51.73 | 44.92 | 47.80 | 50.07 | 46.32 | 33.76 | 56.42 | 55.45 | 60.59 | 39.94 | 63.40 | 47.11 |
EUROSTAT (29. 08. 2022)
| 2019[Mortality rate] | |
|---|---|
| Finland | 32.97 |
| Latvia | 39.14 |
| Lithuania | 41.46 |
| Estonia | 43.74 |
| Slovenia | 52.38 |
| Croatia | 56.10 |
| Sweden | 59.13 |
| France | 59.14 |
| Austria | 59.79 |
| Bolgaria | 60.22 |
| Italy | 67.28 |
| Germany | 70.47 |
| Slovakia | 78.55 |
| Netherlands | 79.26 |
| EU | 79.73 |
| Poland | 81.68 |
| Luxembourg | 83.74 |
| Czech Republic | 86.42 |
| Spain | 87.83 |
| Hungry | 89.11 |
| Romania | 96.42 |
| Greece | 99.36 |
| Belgium | 102.71 |
| Portugal | 105.33 |
| Ciprus | 106.32 |
| Denmark | 112.36 |
| Malta | 112.52 |
| Ireland | 115.47 |
| United Kingdom | 134.47 |
Slovenian Environment Agency, 2015 (1. 09. 2020)
| Number of deaths[number of deaths] | Total mortality in existing pollution[number of deaths] | Reduction of total mortality (%) if PM2,5 pollution was lower than 5 µg/m3[proportion] | Life extension (in years) if PM2,5 pollution was lower than 5 µg/m3[years] | Reduction of total mortality (%) if PM2,5 pollution was lower than 10 µg/m3[proportion] | Life extension (in years) if PM2,5 pollution was lower than 10 µg/m3[years] | |
|---|---|---|---|---|---|---|
| Celje | 440 | 12.90 | 3 | 0.30 | 6.60 | 0.80 |
| Kranj | 415 | 11.20 | 2.90 | 0.30 | 4.60 | 0.60 |
| Ljubljana | 2255 | 11.90 | 2.90 | 0.40 | 4.70 | 0.60 |
| Maribor | 1227 | 15.60 | 2.90 | 0.30 | 5.90 | 0.70 |
| Murska Sobota | 217 | 15.60 | 2.80 | 0.30 | 5.50 | 0.60 |
| Nova Gorica | 337 | 14.80 | 3 | 0.30 | 4.20 | 0.50 |
| Novo mesto | 320 | 13.40 | 2.80 | 0.30 | 5.60 | 0.60 |
| Hrastnik | 102 | 14.60 | 12.90 | 0.40 | 3.90 | 0.50 |
| Trbovlje | 183 | 15.10 | 2.70 | 0.30 | 7.10 | 0.80 |
| Zagorje | 190 | 16.50 | 2.60 | 0.30 | 6.80 | 0.90 |
| Koper | 399 | 12.50 | 2.80 | 0.30 | 3.80 | 0.30 |
| Velenje | 245 | 11.90 | 2.90 | 0.20 | 3.30 | 0.20 |
Goals
- Measures to promote efficient energy use and renewable energy sources in heating of buildings (district heating and gas supply; measures in the field of household heating devices; local energy concepts; provision of information and encouragement of the reduction of heat loss in buildings; accurate register of small combustion installations).
- Measures in the field of transport (Implementation of transport policies in cities – more walking and cycling, increased use of public transport, restrictions on the use of cars; traffic management on state roads and in city areas; measures to reduce pollution from vehicles used in public passenger transport, public utility services and city administration by introducing cleaner vehicles; promotion of electric mobility.
- Measures in other fields (introduction of environmental management systems; reduction of fugitive emissions; reduction of dust from landfills, construction sites and road surfaces of corporate entities; expanding green areas in cities; setting up an air quality website; education/raising awareness about air quality).
Comment
In Slovenia, mortality due to respiratory diseases decreased in 2017–2021 (47 / 100,000) compared to 2012–2016 (63 / 100,000). In the last two years we have to consider mortality due to COVID-19, which is the reason for lower mortality due to respiratory diseases (Ugarte et al 2022) . Reduced mortality in 2020 and 2021 was recorded in all statistical regions (except in Southeast Slovenia in 2020).
If we were to reduce air pollution with PM10 and / or PM2.5 particles by 5 µg / m3 and 10 µg / m3, respectively, these changes would be most reflected in Hrastnik, Zagorje and Trbovlje, which is logical, as these three regions are the most polluted by ambient air pollutants. In other regions, life expectancy would increase by around 0.3 years and mortality would decrease by an average of 3% with a decrease in PM2.5 by 5 µg / m3. Reducing PM2.5 by 10 µg / m3 would increase life expectancy by an average of 0.6 years and reduce mortality by an average of 4.5%.
Respiratory diseases represent more than 6 % of the global burden of disease and cause more deaths and disability than all malign diseases combined, representing 13 % of all hospitalisations. Respiratory diseases can be caused by risk factors such as polluted air, cramped living conditions and poor housing quality. Research has shown that long-term exposure to polluted air increases the likelihood of developing respiratory diseases, such as allergies, asthma, chronic obstructive pulmonary disease (COPD) and lung cancer, especially in children and among the elderly (National Institute of Environmental Health Sciences, 2007).
High prevalence of smoking (environmental pollution with tobacco smoke) and low vaccination rate coverage against influenza and pneumococcal infections are also important factors for mortality due to respiratory diseases. Some of the above-mentioned factors are closely related to socio-economic deprivation. In addition, poverty is related to a twenty-fold increase in relative burden of lung infections that affect very young and very old segments of populations (Steward, Sounders, Kamm, 2008). Studies carried out in European countries have shown that children from low-income families are twice as likely to be exposed to tobacco smoke than children from higher-income families (UN Regional Information Centre for Western Europe, 2010). An epidemiological study carried out in England showed that the increased hospitalisation due to respiratory diseases is closely associated with inequity (Hawker et al., 2003). Poor living conditions, including insufficient heating, poor aeration and cramped conditions, are among the main risk factors for respiratory diseases as well. Poor insulation contributes to a higher mortality rate due to respiratory diseases in wintertime (Clinch, Healy, 2000). Poor aeration and cramped conditions cause the spread of respiratory diseases, such as influenza and tuberculosis, thus increasing the burden of respiratory diseases.
Mortality due to respiratory diseases in Europe is decreasing. Such a pattern occurred in many countries with a high mortality rate, such as Ireland and England. Nevertheless, the rate in these countries remains considerably higher than in other parts of Europe. It has been established that Ireland has one of the highest winter mortality rates (Healy, 2002). Extreme weather conditions cause the aggravation of respiratory diseases, such as asthma and pneumonia, although this can also be a consequence of other factors, such as hypothermia or poor housing conditions. Mortality due to respiratory diseases is closely associated to polluted air and fine particulate matter, including sulphates, in concentrations above 74 µg/m3 (WHO, 2006). A study conducted in England showed that a 10 µg/m3 increase in sulphur dioxide in outdoor air was associated with a 102 % increase in the risk of infant deaths (Hajat, Armstrong et al, 2007). In 1999, a Council Directive relating to limit values for sulphur dioxide, nitrogen dioxide and oxides of nitrogen, particulate matter and lead in ambient air was adopted (Council Directive, 1999). Consequently, a decrease in mortality rates from 62.9/100,000 inhabitants in 1999 to 53.9/100,000 inhabitants in 2001 was recorded. Although this decrease may be a result of other factors, implementation of the Directive is the most likely reason.
Methodology
- ARSO - Agencija RS za okolje, 2015. Kakovost zraka v Sloveniji v letu 2014. Ljubljana, ARSO. Dostopno na: http://www.arso.gov.si/zrak/kakovost%20zraka/poro%C4%8Dila%20in%20publikacije/porocilo_2014.pdf
- Clinch JP, Healy JD, 2000. Housing standards and excess winter mortality. J Epidemiol Community Health 2000; 54:719-720.
- Council Directive 1999/30/EC of 22 April 1999 relating to limit values for sulphur dioxide, nitrogen and oxides of nitrogen, particulate matter and lead in ambient air. Dostopno na: http://eur-lex.europa.eu/legal-content/SL/TXT/PDF/?uri=CELEX:31999L0030…. (accessed 7. Oct. 2016).
- Directives 2008/50/EC of the European Parliament and of the Council of 21 May 2008 on ambient air quality and cleaner air for Europe. Official Journal of the European Union, Vol. 51, 11 June 2008. Dostopno na: http://eur-lex.europa.eu/legal-content/SL/TXT/PDF/?uri=CELEX:32008L0050&from=EN.
- EUROSTAT, 2022. Causes of death statistics - standardised death rate by NUTS 2 region of residence. Dostopno na: https://ec.europa.eu/eurostat/databrowser/view/HLTH_CD_ASDR2__custom_3269698/settings_1/table?lang=en
- Hajat S, Armstrong B, Wilkinson P, Busby A, Dolk H, 2007. Outdoor air pollution and infant mortality: analysis of daily time-series data in Ten English Cities. J Epidemiol Community Health 61:719- 22.
- Hawker JI, Olowokure B, Sufi F, Weinberg J, Gill N, Wilson RC, 2003. Social deprivation and hospital admission for respiratory infection: an ecological study. Respiratory Medicine 97 (11): 1219-1224.
- Healy JD, 2002. Excess winter mortality in Europe: a cross country analysis identifying key risk factors. J Epidemiol Community Health 2003;57:784-789.
- NIJZ - Nacionalni inštitut za javno zdravje, 2013-2022. Zdravniško poročilo o umrli osebi. Ljubljana, NIJZ.
- NIEHS - National Institute of Environmental Health Sciences, 2007. Air pollution and Respiratory diseases.
- SURS - Statistični urad Republike Slovenije, 2013-2022. Prebivalstvo po statističnih regijah. Ljubljana, SURS.
- Stewart L, Saunders P, Kemm J, 2008. Children‘s Environment and Health Action Plan (CEHAP): Pilot Environmental Health Indicators ToolkitConsultation Document
- United Nations Regional Information Centre for Western Europe (2010). Twenty years of environmental and health in Europe: trends and gaps. Dostopno na: http://www.euro.who.int/__data/assets/pdf_file/0013/103513/544E_FS-ParmaOpening.pdf?ua=1.
- Vlada RS, 2009. Operativni program varstva zunanjega zraka pred onesnaževanjem s PM10 (Vlada RS; EVA2009-2511-0021), z dne 3. 11. 2009. Dostopno na: http://www.mop.gov.si/fileadmin/mop.gov.si/pageuploads/zakonodaja/varstvo_okolja/operativni_programi/op_onesnazevanje_pm10.pdf.
- Ugarte MP, Achilleos S, Quattrocchi A, et al. Premature mortality attributable to COVID-19: potential years of life lost in 17 countries around the world, January-August 2020. BMC Public Health. 2022;22(1):54. Published 2022 Jan 9. doi:10.1186/s12889-021-12377-1
- WHO – World Health Organization, 2006. Air quality guidelines. Global update 2005. Particulate matter, ozone, nitrogen dioxide and sulfur dioxide. Dostopno na: http://www.euro.who.int/__data/assets/pdf_file/0005/78638/E90038.pdf.
- Zakon o zbirkah podatkov s področja zdravstvenega varstva. Uradni list RS, št. 65/00, 47/15 in 31/18.